Abstract
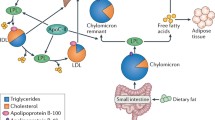
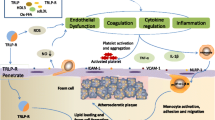
Hypertriglyceridemia is a prevalent risk factor for cardiovascular disease (CVD) and increasingly important in the setting of current obesity and insulin resistance epidemics. High triglyceride (TG) levels are markers for several types of atherogenic lipoproteins. Patients who have hypertriglyceridemia may be at significant risk for CVD even if low-density lipoprotein cholesterol levels are at goal, and therefore warrant treatment that optimizes diet, reduces overweight, and promotes regular exercise. High-risk patients with hypertriglyceridemia, such as those with diabetes, CVD, or metabolic syndrome, may benefit from additional drug treatment aside from a statin to address other lipid abnormalities. In this discussion, we review the role of hypertriglyceridemia and its associated atherogenic lipoproteins in the pathogenesis of atherosclerosis, the relevance of a high TG level as a predictor of CVD, the cardiovascular outcomes from TG-lowering intervention trials, and the current guidelines for treating hypertriglyceridemia.
Similar content being viewed by others
Abbreviations
- ACCORD:
-
Action to Control Cardiovascular Risk in Diabetes
- AIM-HIGH:
-
Atherothrombosis Intervention in Metabolic syndrome with Low HDL/High Triglycerides: Impact on Global Health Outcomes
- JELIS:
-
Japan EPA Lipid Intervention Study
- NCEP ATP III:
-
National Cholesterol Education Program Adult Treatment Panel III
- NHANES:
-
National Health and Nutrition Examination Survey
- PROVE IT-TIMI 22:
-
Pravastatin or Atorvastatin Evaluation and Infection Therapy-Thrombolysis in Myocardial Infarction 22
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Lloyd-Jones D, Adams RJ, Brown TM, et al. Heart disease and stroke statistics–2010 update: a report from the American Heart Association. Circulation. 2010;121(7):e46–e215.
National Cholesterol Education Program (NCEP) Expert Panel on Detection. Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III): Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). Circulation. 2002;106(25):3143–421.
Ford ES, Giles WH, Dietz WH. Prevalence of the metabolic syndrome among US adults: findings from the third National Health and Nutrition Examination Survey. JAMA. 2002;287(3):356–9.
Alexander CM, Landsman PB, Teutsch SM, et al. NCEP-defined metabolic syndrome, diabetes, and prevalence of coronary heart disease among NHANES III participants age 50 years and older. Diabetes. 2003;52(5):1210–4.
Hokanson JE, Austin MA. Plasma triglyceride level is a risk factor for cardiovascular disease independent of high-density lipoprotein cholesterol level: a meta-analysis of population-based prospective studies. J Cardiovasc Risk. 1996;3(2):213–9.
Schulte H, Cullen P, Assmann G. Obesity, mortality and cardiovascular disease in the Münster Heart Study (PROCAM). Atherosclerosis. 1999;144(1):199–209.
Sarwar N, Danesh J, Eiriksdottir G, et al. Triglycerides and the risk of coronary heart disease: 10,158 incident cases among 262,525 participants in 29 Western prospective studies. Circulation. 2007;115:450–8.
Baigent C, Keech A, Kearney PM, et al. Cholesterol Treatment Trialists Collaborators. Efficacy and safety of cholesterol-lowering treatment: prospective meta-analysis of data from 90,056 participants in 14 randomised trials of statins. Lancet. 2005;366(9493):1267–78.
Brewer Jr HB. Hypertriglyceridemia: changes in the plasma lipoproteins associated with an increased risk of cardiovascular disease. Am J Cardiol. 1999;83(9B):3F–12F.
Gianturco SH, Ramprasad MP, Song R, et al. Apolipoprotein B-48 or its apolipoprotein B-100 equivalent mediates the binding of triglyceride rich lipoproteins to their unique human monocyte-macrophage receptor. Arterioscler Thromb Vasc Biol. 1998;18(6):968–76.
Botham KM, Moore EH, De Pascale C, et al. The induction of macrophage foam cell formation by chylomicron remnants. Biochem Soc Trans. 2007;35:454–8.
Ooi EM, Barrett PH, Chan DC, et al. Apolipoprotein C-III: understanding an emerging cardiovascular risk factor. Clin Sci. 2008;114(10):611–24.
Zheng C, Furtado J, Khoo C, et al. Apolipoprotein C-III and the metabolic basis for hypertriglyceridemia and the dense LDL phenotype. Circulation. 2010;121(15):1722–34. These results support a central role for apo C-III in metabolic defects leading to hypertriglyceridemia and the dense LDL phenotype. In hypertriglyceridemia, TG-rich lipoprotein metabolism shifts from an apo E–dominated system to an apo C-III–dominated system characterized by reduced clearance of TG-rich lipoproteins and their conversion to dense LDL.
Kamagate A, Dong HH. FoxO1 integrates insulin signaling to VLDL production. Cell Cycle. 2008;7(20):3162–70.
Cooper AD. Hepatic uptake of chylomicron remnants. J Lipid Res. 1997;38(11):2173–92.
Colhoun HM, Otvos JD, Rubens MB, et al. Lipoprotein subclasses and particle sizes and their relationship with coronary artery calcification in men and women with and without type 1 diabetes. Diabetes. 2002;51(6):1949–56.
Van Eck M, Zimmermann R, Groot PH, et al. Role of macrophage-derived lipoprotein lipase in lipoprotein metabolism and atherosclerosis. Arterioscler Thromb Vasc Biol. 2000;20(9):E53–62.
Kawakami A, Osaka M, Tani M, et al. Apolipoprotein CIII links hyperlipidemia with vascular endothelial function. Circulation. 2008;118(7):731–42.
Wang L, Gill R, Pedersen TL, et al. Triglyceride-rich lipoprotein lipolysis releases neutral and oxidized FFAs that induce endothelial cell inflammation. J Lipid Res. 2009;50(2):204–13.
Palmer AM, Murphy N, Graham A. Triglyceride-rich lipoproteins inhibit cholesterol efflux to apolipoprotein (apo) A1 from human macrophage foam cells. Atherosclerosis. 2004;173(1):27–38.
Patel S, Puranik R, Nakhla S, et al. Acute hypertriglyceridaemia in humans increases the triglyceride content and decreases the anti-inflammatory capacity of high density lipoproteins. Atherosclerosis. 2009;204(1):424–8.
Kawakami A, Aikawa M, Alcaide P, et al. Apolipoprotein CIII induces expression of vascular cell adhesion molecule-1 in vascular endothelial cells and increases adhesion of monocytic cells. Circulation. 2006;114(7):681–7.
Hiukka A, Stahlman M, Pettersson C, et al. ApoCIII-Enriched LDL in type 2 diabetes displays altered lipid composition, increased susceptibility for sphingomyelinase, and increased binding to biglycan. Diabetes. 2009;58(9):2018–26.
Pollin TI, Damcott CM, Shen H, et al. A null mutation in human APOC3 confers a favorable plasma lipid profile and apparent cardioprotection. Science. 2008;322(5908):1702–5.
Zheng C, Murdoch S, Brunzell J, et al. Lipoprotein lipase bound to apolipoprotein B lipoproteins accelerates clearance of postprandial lipoproteins in humans. Arterioscler Thromb Vasc Biol. 2006;26(4):891–6.
Goldberg IJ. Lipoprotein lipase and lipolysis: central roles in lipoprotein metabolism and atherogenesis. J Lipid Res. 1996;37(4):693–707.
Olivecrona G, Olivecrona T. Triglyceride lipases and atherosclerosis. Curr Opin Lipidol. 2010;21:409–15.
Wehinger A, Tancevski I, Schgoer W, et al. Phospholipid transfer protein augments apoptosis in THP-1-derived macrophages induced by lipolyzed hypertriglyceridemic plasma. Arterioscler Thromb Vasc Biol. 2007;27:908–15.
Georgieva AM, Cate HT, Keulen ET, et al. Prothrombotic markers in familial combined hyperlipidemia: evidence of endothelial cell activation and relation to metabolic syndrome. Atherosclerosis. 2004;75(2):345–51.
Sutherland JP, McKinley B, Eckel RH. The metabolic syndrome and inflammation. Metab Syndr Relat Disord. 2004;2(2):82–104.
Norata GD, Grigore L, Raselli S, et al. Post-prandial endothelial dysfunction in hypertriglyceridemic subjects: molecular mechanisms and gene expression studies. Atherosclerosis. 2007;193:321–7.
Jacobs DR, Barrett-Connor E. Retest reliability of plasma cholesterol and triglyceride: the Lipid Research Clinics Prevalence Study. Am J Epidemiol. 1982;116:878–85.
Asia Pacific Cohort Studies Collaboration. Serum triglycerides as a risk factor for cardiovascular diseases in the Asia-Pacific region. Circulation. 2004;110:2678–86.
Di Angelantonio E, Sarwar N, Perry P, et al. Emerging risk factors collaboration. Major lipids, apolipoproteins, and risk of vascular disease. JAMA. 2009;302:1993–2000.
• Carey VJ, Bishop L, Laranjo N, et al. Contribution of high plasma triglycerides and low high-density lipoprotein cholesterol to residual risk of coronary heart disease after establishment of low-density lipoprotein cholesterol control. Am J Cardiol. 2010;106:757–63. This study highlights a strong and synergistic contribution of high TG and low HDL-C levels to CHD when LDL-C is at goal. These results suggest that lowering TGs may have greater potential for clinical benefit when LDL-C is low.
• Assmann G, Cullen P, Schulte H. Non-LDL-related dyslipidaemia and coronary risk: a case–control study. Diab Vasc Dis Res. 2010;7(3):204–12. Findings from this study suggest that residual cardiovascular risk associated with hypertriglyceridemia is greatest in persons in whom LDL-C concentration is in a low _target range.
Sacks FM, Tonkin AM, Craven T, et al. Coronary heart disease in patients with low LDL-cholesterol: benefit of pravastatin in diabetics and enhanced role for HDL-cholesterol and triglycerides as risk factors. Circulation. 2002;105:1424–8.
Miller M, Cannon CP, Murphy SA, et al. Impact of triglyceride levels beyond low-density lipoprotein cholesterol after acute coronary syndrome in the PROVE IT-TIMI 22 trial. J Am Coll Cardiol. 2008;51:724–30.
Miller M, Stone NJ, Ballantyne C, et al. Triglycerides and cardiovascular disease: a scientific statement from the american heart association. Circulation. 2011;123:2292–333.
Nordestgaard BG, Benn M, Schnohr P, et al. Nonfasting triglycerides and risk of myocardial infarction, ischemic heart disease, and death in men and women. JAMA. 2007;298:299–308.
Bansal S, Buring JE, Rifai N, et al. Fasting compared with nonfasting triglycerides and risk of cardiovascular events in women. JAMA. 2007;298:309–16.
Miller M, Ginsberg HN, Schaefer EJ. Relative atherogenicity and predictive value of non-high-density lipoprotein cholesterol for coronary heart disease. Am J Cardiol. 2008;101:1003–8.
Thompson A, Danesh J. Associations between apolipoprotein B, apolipoprotein AI, the apolipoprotein B/AI ratio and coronary heart disease: a literature-based meta-analysis of prospective studies. J Intern Med. 2006;259(5):481–92.
Pischon T, Girman CJ, Sacks FM, et al. Non-high-density lipoprotein cholesterol and apolipoprotein B in the prediction of coronary heart disease in men. Circulation. 2005;112:3375–83.
Sniderman A, Williams K, Cobbaert C. ApoB versus non-HDL-C: what to do when they disagree. Curr Atheroscler Rep. 2009;11:358–63.
Barter PJ, Ballantyne CM, Carmena R, et al. Apo B versus cholesterol in estimating cardiovascular risk and in guiding therapy: report of the thirty-person/ten-country panel. J Intern Med. 2006;259:247–58.
Stein EA, Lane M, Laskarzewski P. Comparison of statins in hypertriglyceridemia. Am J Cardiol. 1998;81:66B–9B.
Sacks FM, Alaupovic P, Moye LA. Effect of pravastatin on apolipoproteins B and C-III in very-low-density lipoproteins and low-density lipoproteins. Am J Cardiol. 2002;90(2):165–7.
Girman CJ, Rhodes T, Mercuri M, et al. 4S Group and the AFCAPS/TexCAPS Research Group. The metabolic syndrome and risk of major coronary events in the Scandinavian Simvastatin Survival Study (4S) and the Air Force/Texas Coronary Atherosclerosis Prevention Study (AFCAPS/TexCAPS). Am J Cardiol. 2004;93:136–41.
Pyörälä K, Pedersen TR, Kjekshus J, et al. Cholesterol lowering with simvastatin improves prognosis of diabetic patients with coronary heart disease: a subgroup analysis of the Scandinavian Simvastatin Survival Study (4S) [published correction appears in Diabetes Care. 1997;20:1048]. Diabetes Care. 1997;20:614–20.
Sacks FM, Alaupovic P, Moye LA, et al. VLDL, apolipoproteins B, CIII, and E, and risk of recurrent coronary events in the Cholesterol and Recurrent Events (CARE) trial. Circulation. 2000;102:1886–92.
Kastelein JJP, van der Stieg W, Holme I, et al. Lipids, apolipoproteins, and their ratios in relation to cardiovascular events with statin treatment. Circulation. 2008;117:3002–9.
Pfeffer MA, Sacks FM, Moyé LA, et al. Influence of baseline lipids on effectiveness of pravastatin in the CARE Trial: cholesterol and recurrent events. J Am Coll Cardiol. 1999;33:125–30.
Ginsberg HN, Elam MB, Lovato LC, et al. Effects of combination lipid therapy in type 2 diabetes mellitus. The ACCORD Study Group. N Engl J Med. 2010;362:1563–74.
Scott R, O’Brien R, Fulcher G, et al. Effects of fenofibrate treatment on cardiovascular disease risk in 9,795 individuals with type 2 diabetes and various components of the metabolic syndrome: the Fenofibrate Intervention and Event Lowering in Diabetes (FIELD) study. Diabetes Care. 2009;32:493–8.
The BIP Study Group. Secondary prevention by raising HDL cholesterol and reducing triglycerides in patients with coronary artery disease: the Bezafibrate Infarction Prevention (BIP) study. Circulation. 2000;102:21–7.
Manninen V, Tenkanen L, Koskinen P, et al. Joint effects of serum triglyceride and LDL cholesterol and HDL cholesterol concentrations on coronary heart disease risk in the Helsinki Heart Study: implications for treatment. Circulation. 1992;85:37–45.
Robins SJ, Collins D, Wittes JT, et al. Relation of gemfibrozil treatment and lipid levels with major coronary events: VA-HIT: a randomized controlled trial. JAMA. 2001;285:1585–91.
Tenkanen L, Mantarri M, Manninen V. Some coronary risk factors related to the insulin resistance syndrome and treatment with gemfibrozil: experience from the Helsinki Heart Study. Circulation. 1995;92:1779–85.
Rubins HB, Robins SJ, Collins D, et al. Diabetes, plasma insulin, and cardiovascular disease: subgroup analysis from the Department of Veterans Affairs high-density lipoprotein intervention trial (VA-HIT). Arch Intern Med. 2002;162:2597–604.
Tenenbaum A, Motro M, Fisman EZ, et al. Bezafibrate for the secondary prevention of myocardial infarction in patients with metabolic syndrome. Arch Intern Med. 2005;165:1154–60.
Scott R, d’Emden M, Best J, et al. (on behalf of the FIELD Investigators).: Features of metabolic syndrome identify individuals with type 2 diabetes mellitus at high risk for cardiovascular events and greater absolute benefits of fenofibrate. Circulation. 2007;116:II_838. Abstract 3691.
Sacks FM, Carey VJ, Fruchart JC. Combination lipid therapy in type 2 diabetes. N Engl J Med. 2010;363(7):692. author reply 694–5. Meta-analysis of the major clinical trials of fibrate treatment found that fibrates reduced CHD events among patients with hypertriglyceridemia and low HDL-C.
• Jun M, Foote C, Lv J, et al. Effects of fibrates on cardiovascular outcomes: a systematic review and meta-analysis. Lancet. 2010;375(9729):1875–84. This reference is important because it reviews inconsistent findings from several clinical trials regarding the effect of fibrates on cardiovascular risk concluding that fibrates can reduce the risk of major coronary events, and might have a role in individuals at high risk of cardiovascular events and in those with combined dyslipidemia.
Kamanna VS, Kashyap ML. Mechanism of action of niacin. Am J Cardiol. 2008;101:20B–6B.
Coronary Drug Project Research Group. Clofibrate and niacin in coronary heart disease. JAMA. 1975;231:360–81.
Canner PL, Berge KG, Wenger NK, et al. Fifteen year mortality in coronary drug project patients: long-term benefit with niacin. J Am Coll Cardiol. 1986;8:1245–55.
AIM-HIGH Investigators. The role of niacin in raising high-density lipoprotein cholesterol to reduce cardiovascular events in patients with atherosclerotic cardiovascular disease and optimally treated low-density lipoprotein cholesterol Rationale and study design. The Atherothrombosis Intervention in Metabolic syndrome with low HDL/high triglycerides: Impact on Global Health outcomes (AIM-HIGH). Am Heart J. 2011;161(3):471–7.
Harris WS, Miller M, Tighe AP, et al. Omega-3 fatty acids and coronary heart disease risk: clinical and mechanistic perspectives. Atherosclerosis. 2008;197:12–24.
Balk E, Chung M, Lichtenstein A, et al. Effects of Omega-3 Fatty Acids on CardiovascularRisk Factors and Intermediate Markers of Cardiovascular Disease. Evidence Report/Technology Assessment No. 93 (prepared byTufts-New England Medical Center Evidence-Based Practice Center under contract No. 290-02-0022). AHRQ publication No. 04-E010-2. Rockville, MD: Agency for Healthcare Research and Quality; 2004.
Kris-Etherton PM, Harris WS, Appel LJ. American Heart Association Nutrition Committee. Fish consumption, fish oil, omega-3 fatty acids, and cardiovascular disease [published correction appears in Circulation 2003,107:512]. Circulation. 2002;106:2747–57.
Marik PE, Varon J. Omega-3 dietary supplements and the risk of cardiovascular events: a systematic review. Clin Cardiol. 2009;32(7):365–72.
Yokoyama M, Origasa H, Matsuzaki M, et al. Japan EPA Lipid Intervention Study (JELIS) Investigators. Effects of eicosapentaenoic acid on major coronary events in hypercholesterolaemic patients (JELIS): a randomised open-label, blinded endpoint analysis. Lancet. 2007;369:1090–8.
Fox CS, Massaro JM, Hoffmann U, et al. Abdominal visceral and subcutaneous adipose tissue compartments: association with metabolic risk factors in the Framingham Heart Study. Circulation. 2007;116:39–48.
Sacks FM, Bray GA, Carey VJ, et al. Comparison of weight-loss diets with different compositions of fat, protein, and carbohydrates. N Engl J Med. 2009;360:859–73.
Appel LJ, Sacks FM, Carey VJ, OmniHeart Collaborative Research Group, et al. Effects of protein, monounsaturated fat, and carbohydrate intake on blood pressure and serum lipids: results of the OmniHeart randomized trial. JAMA. 2005;294:2455–64.
Durstine JL, Grandjean PW, Cox CA, Thompson PD. Lipids, lipoproteins and exercise. J Cardiopulm Rehabil. 2002;22:385–98.
Fruchart JC, Sacks FM, Hermans MP, et al. Residual Risk Reduction Initiative (R3I). The Residual Risk Reduction Initiative: a call to action to reduce residual vascular risk in dyslipidaemic patient. Diab Vasc Dis Res. 2008;5(4):319–35.
Poobalan A, Aucott L, Smith WC, et al. Effects of weight loss in overweight/obese individuals and long-term lipid outcomes: a systematic review. Obes Rev. 2004;5:43–50.
Brown B, Canner PL, McGovern ME, et al. Nicotinic acid. In: Ballantyne C, editor. Clinical lipidology, a companion to braunwald’s heart disease. Philadelphia: Saunders; 2009. p. 298–314.
Jones PH. Fibrates. In: Ballantyne C, editor. Clinical lipidology, a companion to braunwald’s heart disease. Philadelphia: Saunders; 2009. p. 315–25.
Harris WS, Jacobson TA. Omega-3 fatty acids. In: Ballantyne C, editor. Clinical lipidology, a companion to braunwald’s heart disease. Philadelphia: Saunders; 2009. p. 326–38.
Fontana L, Villareal DT, Weiss EP, the Washington University School of Medicine CALERIE Group, et al. Calorie restriction or exercise: effects on coronary heart disease risk factors: a randomized, controlled trial. Am J Physiol Endocrinol Metab. 2007;293:E197–202.
Ridker PM, Danielson E, Fonseca FA, et al. JUPITER Study Group. Rosuvastatin to prevent vascular events in men and women with elevated C-reactive protein. N Engl J Med. 2008;359:2195–207.
Disclosure
Conflicts of interest: B.G. Talayero: none; F.M. Sacks: has board membership with R3i Foundation; has been a consultant for Abbott, Amgen, Pfizer, Roche, Merck, Eli Lilly, ISIS, and Genzyme; has given expert testimony for Abbott and Par; has received grant support from ISIS; and has received honoraria from Abbott.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Talayero, B.G., Sacks, F.M. The Role of Triglycerides in Atherosclerosis. Curr Cardiol Rep 13, 544–552 (2011). https://doi.org/10.1007/s11886-011-0220-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11886-011-0220-3