Leveraging Personal Technologies in the Treatment of Schizophrenia Spectrum Disorders: Scoping Review
- PMID: 39348196
- PMCID: PMC11474131
- DOI: 10.2196/57150
Leveraging Personal Technologies in the Treatment of Schizophrenia Spectrum Disorders: Scoping Review
Abstract
Background: Digital mental health is a rapidly growing field with an increasing evidence base due to its potential scalability and impacts on access to mental health care. Further, within underfunded service systems, leveraging personal technologies to deliver or support specialized service delivery has garnered attention as a feasible and cost-effective means of improving access. Digital health relevance has also improved as technology ownership in individuals with schizophrenia has improved and is comparable to that of the general population. However, less digital health research has been conducted in groups with schizophrenia spectrum disorders compared to other mental health conditions, and overall feasibility, efficacy, and clinical integration remain largely unknown.
Objective: This review aims to describe the available literature investigating the use of personal technologies (ie, phone, computer, tablet, and wearables) to deliver or support specialized care for schizophrenia and examine opportunities and barriers to integrating this technology into care.
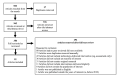
Methods: Given the size of this review, we used scoping review methods. We searched 3 major databases with search teams related to schizophrenia spectrum disorders, various personal technologies, and intervention outcomes related to recovery. We included studies from the full spectrum of methodologies, from development papers to implementation trials. Methods and reporting follow the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines.
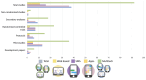
Results: This search resulted in 999 studies, which, through review by at least 2 reviewers, included 92 publications. Included studies were published from 2010 to 2023. Most studies examined multitechnology interventions (40/92, 43%) or smartphone apps (25/92, 27%), followed by SMS text messaging (16/92, 17%) and internet-based interventions (11/92, 12%). No studies used wearable technology on its own to deliver an intervention. Regarding the stage of research in the field, the largest number of publications were pilot studies (32/92, 35%), followed by randomized control trials (RCTs; 20/92, 22%), secondary analyses (16/92, 17%), RCT protocols (16/92, 17%), development papers (5/92, 5%), and nonrandomized or quasi-experimental trials (3/92, 3%). Most studies did not report on safety indices (55/92, 60%) or privacy precautions (64/92, 70%). Included studies tend to report consistent positive user feedback regarding the usability, acceptability, and satisfaction with technology; however, engagement metrics are highly variable and report mixed outcomes. Furthermore, efficacy at both the pilot and RCT levels report mixed findings on primary outcomes.
Conclusions: Overall, the findings of this review highlight the discrepancy between the high levels of acceptability and usability of these digital interventions, mixed efficacy results, and difficulties with sustained engagement. The discussion highlights common patterns that may underscore this observation in the field; however, as this was a scoping review, a more in-depth systematic review or meta-analysis may be required to better understand the trends outlined in this review.
Keywords: acceptability; access to specialized resources; care; clinical integration; database; digital health; digital mental health; eHealth; efficacy; engagement; feasibility; health technology; mental health; mental health care; mobile phone; mood disorder; mood disorders; neurodevelopment; personal technology; satisfaction; schizophrenia; schizophrenia spectrum disorder; scoping review; specialized care; support; technology; text; text messaging; usability; user feedback.
©Jessica D'Arcey, John Torous, Toni-Rose Asuncion, Leah Tackaberry-Giddens, Aqsa Zahid, Mira Ishak, George Foussias, Sean Kidd. Originally published in JMIR Mental Health (https://mental.jmir.org), 30.09.2024.
Conflict of interest statement
Conflicts of Interest: JT is the editor in chief of
Figures
Similar articles
-
Folic acid supplementation and malaria susceptibility and severity among people taking antifolate antimalarial drugs in endemic areas.Cochrane Database Syst Rev. 2022 Feb 1;2(2022):CD014217. doi: 10.1002/14651858.CD014217. Cochrane Database Syst Rev. 2022. PMID: 36321557 Free PMC article.
-
Attributes, Methods, and Frameworks Used to Evaluate Wearables and Their Companion mHealth Apps: Scoping Review.JMIR Mhealth Uhealth. 2024 Apr 5;12:e52179. doi: 10.2196/52179. JMIR Mhealth Uhealth. 2024. PMID: 38578671 Free PMC article. Review.
-
The Use of Technology to Provide Mental Health Services to Youth Experiencing Homelessness: Scoping Review.J Med Internet Res. 2023 Jan 16;25:e41939. doi: 10.2196/41939. J Med Internet Res. 2023. PMID: 36645703 Free PMC article. Review.
-
Longitudinal Coadaptation of Older Adults With Wearables and Voice-Activated Virtual Assistants: Scoping Review.J Med Internet Res. 2024 Aug 7;26:e57258. doi: 10.2196/57258. J Med Internet Res. 2024. PMID: 39110963 Free PMC article. Review.
-
Beyond the black stump: rapid reviews of health research issues affecting regional, rural and remote Australia.Med J Aust. 2020 Dec;213 Suppl 11:S3-S32.e1. doi: 10.5694/mja2.50881. Med J Aust. 2020. PMID: 33314144
References
-
- Wozney L, Mcgrath P, Newton A, Hartling L, Curran J, Huguet A, Rao S. RE-AIMing e-mental health: a rapid review of current research. Mental Health Commission of Canada. 2017. [2024-04-29]. https://www.mentalhealthcommission.ca/wp-content/uploads/drupal/2017-08/... .
-
- Kasckow J, Felmet K, Appelt C, Thompson R, Rotondi A, Haas G. Telepsychiatry in the assessment and treatment of schizophrenia. Clin Schizophr Relat Psychoses. 2014 Apr;8(1):21–7A. doi: 10.3371/CSRP.KAFE.021513. https://europepmc.org/abstract/MED/23428781 9684Q297P151LW04 - DOI - PMC - PubMed
-
- Firth J, Cotter J, Torous J, Bucci S, Firth JA, Yung AR. Mobile phone ownership and endorsement of "mHealth" among people with psychosis: a meta-analysis of cross-sectional studies. Schizophr Bull. 2016 Mar;42(2):448–55. doi: 10.1093/schbul/sbv132. http://europepmc.org/abstract/MED/26400871 sbv132 - DOI - PMC - PubMed
-
- Naslund JA, Aschbrenner KA, Bartels SJ. How people with serious mental illness use smartphones, mobile apps, and social media. Psychiatr Rehabil J. 2016 Dec;39(4):364–7. doi: 10.1037/prj0000207. https://europepmc.org/abstract/MED/27845533 2016-29862-001 - DOI - PMC - PubMed
-
- Ruiz-Martínez I, Esparcia J. Internet access in rural areas: brake or stimulus as post-COVID-19 opportunity? Sustainability. 2020 Nov 18;12(22):9619. doi: 10.3390/su12229619. - DOI
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical